Healing Concussions for lasting results – not just symptom management.
By Dr. Brad DeBeer, Axon Integrative Health – Denver Cherry Creek
Concussions are often discussed as “mild” traumatic brain injuries. In reality, there is nothing mild about the downstream physiological disruption they can create, especially when symptoms linger.
One of the most overlooked systems affected by concussion is the gut.
At Axon Integrative Health, we take a comprehensive brain-body-mind approach. We recognize that every concussion subtype influences the Brain-Gut Axis, and if we fail to address gut dysfunction, inflammation, autonomic imbalance, and metabolic disruption, recovery may stall.
Let’s break this down.
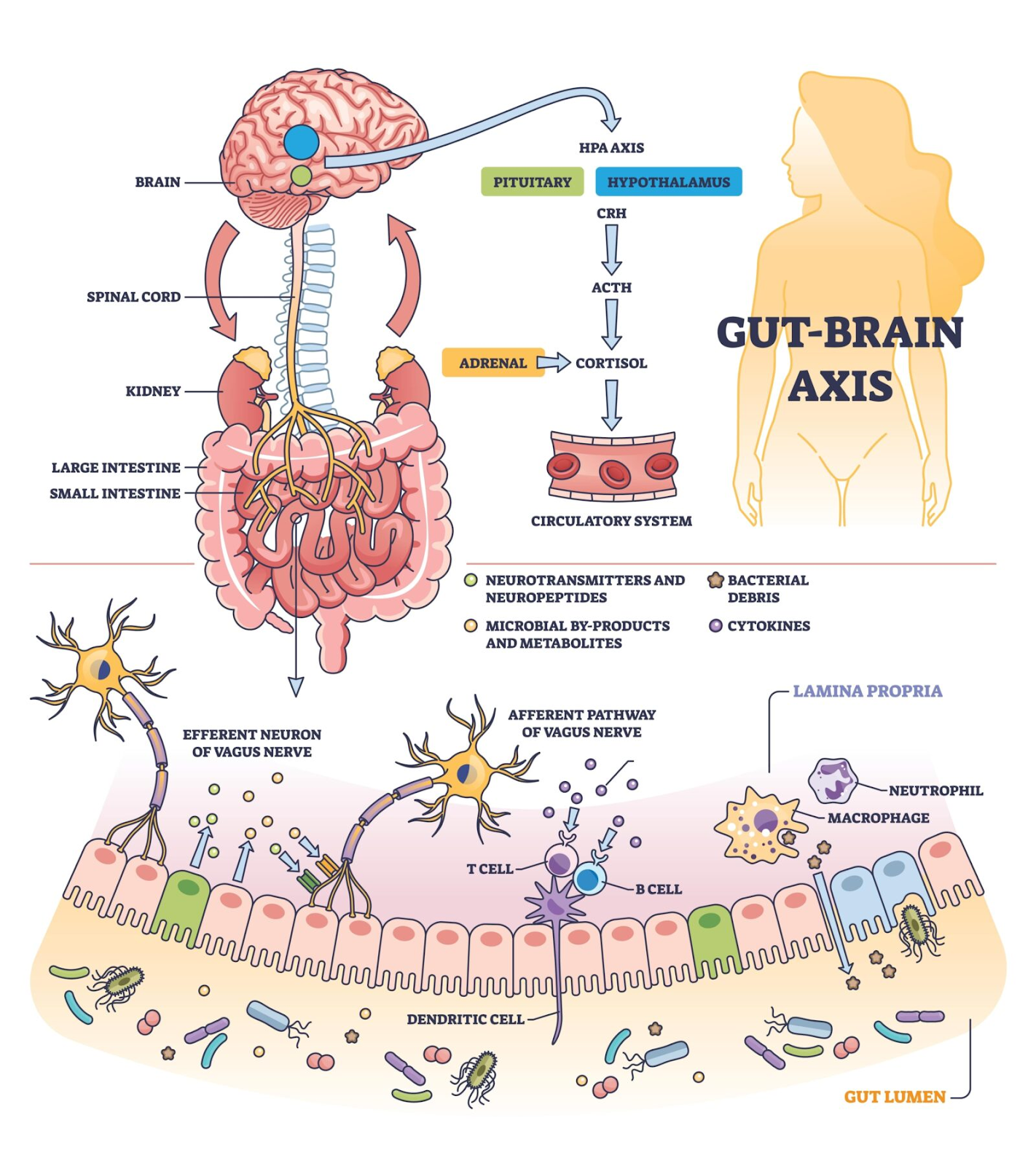
What Is the Brain-Gut Axis?
The Brain–Gut Axis is a bidirectional communication network between the central nervous system and the gastrointestinal system. It involves:
- The autonomic nervous system (sympathetic/parasympathetic balance)
- The vagus nerve
- The enteric nervous system
- The immune system
- The microbiome
- Hormonal signaling (cortisol, thyroid, sex hormones)
After a concussion, dysregulation in one or more of these systems is almost universal.
The result?
- Bloating
- Constipation or diarrhea
- Food sensitivities
- Histamine intolerance
- Brain fog
- Anxiety
- Fatigue
- Poor sleep
- Slower neurological recovery
The gut is not separate from the brain. It is an extension of it. And can help perpetuate symptoms that may feel unrelated to a recent bump to the head.
The 5 Subtypes of Concussions: And How Each Impacts the Gut
At Axon Integrative Health, we categorize concussions into five major subtypes. While patients may present predominantly with one, most experience overlap.
1. VOMS Subtype (Vestibular/Ocular/Motion Sensitivity)
The VOMS subtype refers to dysfunction identified through Vestibular Ocular Motor Screening (VOMS), often used in concussion assessment.
Symptoms include:
- Dizziness
- Nausea
- Light sensitivity
- Motion sensitivity
- Visual tracking problems
When vestibular systems are disrupted, the autonomic nervous system often follows. Persistent nausea and motion sensitivity can impair appetite and digestive rhythm. Chronic vestibular stress also increases sympathetic dominance, reducing vagal tone which is critical for gut motility and secretion.
2. Cervicogenic Subtype
This subtype originates from the upper cervical spine and associated soft tissues.
Symptoms include:
- Headaches
- Neck pain
- Visual disturbances
- Dizziness
- Brain fog
The upper cervical spine has intimate neurological connections with the brainstem and vagus nerve nuclei. When cervical dysfunction persists, it can alter vagal output, impair digestion, and reduce parasympathetic regulation of the gut.
Structural dysfunction → Brainstem irritation → Vagal disruption → Gut dysmotility.
3. Cognitive / Psychological Subtype
Symptoms include:
- Brain fog
- Memory issues
- Mood swings
- Anxiety
- Depression
- Irritability
Regions like the prefrontal cortex, anterior cingulate cortex, and limbic structures are vulnerable after concussion. These areas regulate stress responses and emotional processing.
Chronic stress activation elevates cortisol and alters gut permeability (“leaky gut”), microbiome balance, and inflammatory signaling. The gut then feeds inflammatory cytokines back to the brain-worsening cognition and mood.
It becomes a loop.
4. Autonomic / Blood Flow Subtype
This is one of the most common and under-recognized subtypes.
Symptoms include:
- Exercise intolerance
- Heart rate variability dysfunction
- Lightheadedness
- Fatigue
- Temperature dysregulation
- POTS-like symptoms
Autonomic dysfunction directly impacts digestion. Sympathetic dominance suppresses:
- Gastric acid production
- Enzyme release
- Peristalsis
- Nutrient absorption
Reduced cerebral blood flow also impairs metabolic recovery, increasing oxidative stress systemically… including in the gut lining.
5. Inflammatory / Metabolic / Hormonal Subtype
Concussions initiate a neurometabolic cascade:
- Ionic shifts
- Glutamate excitotoxicity
- Mitochondrial dysfunction
- Oxidative stress
- Neuroinflammation
This inflammatory state extends beyond the brain.
The gut barrier becomes more permeable. Microbiome diversity may decrease. Hormonal disruption (thyroid, cortisol, sex hormones) further alters gut motility and immune regulation.
Inflammation in the brain → inflammation in the gut → amplified systemic symptoms.
The Brain-Gut Axis Is Affected in ALL Concussion Subtypes
Regardless of the primary subtype, every concussion involves:
- Autonomic disruption
- Inflammatory signaling
- Neurotransmitter imbalance
- Hormonal stress response changes
These mechanisms converge at the gut.
If the gut is inflamed, dysbiotic, or hypomotile, recovery slows.
Healing the brain requires healing the gut.
How We Address Concussions and Gut Health at Axon Integrative Health
Our approach is integrative, individualized, and systems-based.
Functional Neurology
We assess brain network dysfunction and create targeted neurorehabilitation programs to restore vestibular, ocular, autonomic, and cortical balance. Improving neurological regulation improves vagal tone and gut signaling.
Acupuncture
Acupuncture modulates autonomic balance, reduces inflammation, and supports vagus nerve activation. It is highly effective for nausea, motility disorders, and stress-related gut dysfunction.
Chiropractic Care
Precise cervical and spinal care improves afferent input to the central nervous system, supporting autonomic regulation and brain-body recalibration.
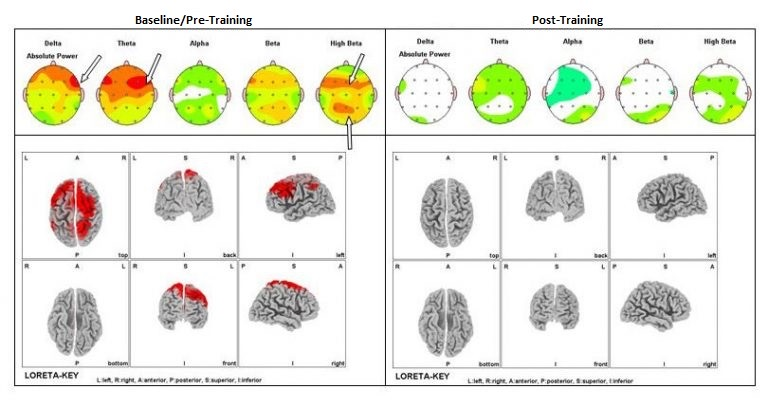
Neurofeedback
Neurofeedback trains dysregulated brainwave patterns associated with anxiety, poor sleep, and stress reactivity, indirectly improving gut function through improved autonomic balance and fuel utilization.
Transcranial Laser Therapy
Transcranial photobiomodulation enhances mitochondrial function, reduces neuroinflammation, and improves cerebral blood flow which is key for metabolic recovery.
IV Therapy
We utilize targeted IV therapies to support:
- Mitochondrial health
- Antioxidant status
- Detoxification pathways
- Nutrient repletion
Optimizing cellular energy supports both brain and intestinal epithelial repair.
Hyperbaric Oxygen Therapy (HBOT)
HBOT enhances oxygen delivery, reduces inflammation, and supports angiogenesis. Improved oxygenation benefits both neural tissue and gut mucosal integrity.
Pulsed Electromagnetic Field Therapy (PEMF)
PEMF supports cellular signaling, reduces inflammation, and enhances recovery at the mitochondrial level.
Vagus Nerve Stimulation
Vagal tone is central to the Brain-Gut Axis. Targeted stimulation improves:
- Heart rate variability
- Digestive motility
- Inflammatory regulation
- Emotional resilience
Lifestyle Management
We guide patients in:
- Anti-inflammatory nutrition
- Blood sugar stabilization
- Sleep optimization
- Breathwork
- Stress reduction
- Graded exercise protocols
Lifestyle is not secondary—it is foundational.
Targeted Supplementation
Based on individual needs, we may incorporate:
- Omega-3 fatty acids
- Magnesium
- Probiotics
- Gut barrier support nutrients
- Mitochondrial cofactors
- Anti-inflammatory compounds
Precision matters.
The Axon Integrative Health Difference
At Axon Integrative Health, we do not treat concussions as isolated brain events.
We evaluate:
- Brain networks
- Cervical integrity
- Autonomic balance
- Metabolic status
- Hormonal function
- Gut health
Because healing requires systems thinking.
If you are struggling with lingering concussion symptoms—brain fog, digestive issues, anxiety, fatigue, exercise intolerance, it may not be “just in your head.”
It may be your Brain-Gut Axis asking for support.
Ready to Start Healing?
If you or a loved one is navigating post-concussion symptoms, our team at Axon Integrative Health in Denver Colorado can help identify your concussion subtype and create a personalized recovery plan that restores both brain and gut function. Whether you’re a local, or would be traveling to see us, we will build a customized plan to help you reach your goals.
Your brain and gut are connected.
Let’s treat them that way.




