A Systems-Based Approach to Complex Chronic Illness in Denver CO
By Dr. Brad DeBeer, Axon Integrative Health
If you have been diagnosed with Dysautonomia, POTS, or MCAS, you likely know the frustration of fragmented care.
You may have been told:
- “Your labs are normal.”
- “It’s anxiety.”
- “Just increase salt and fluids.”
- “Avoid your triggers.”
While these recommendations can be helpful, they often fail to address the deeper physiology.
At Axon Integrative Health, we view these conditions through four interconnected lenses:
- Functional Neurology
- Functional Medicine
- Physical Medicine
- Human Performance
Because Dysautonomia, POTS, and MCAS are not isolated diagnoses.
They are systems miscommunications.
Understanding the Conditions
What Is Dysautonomia?
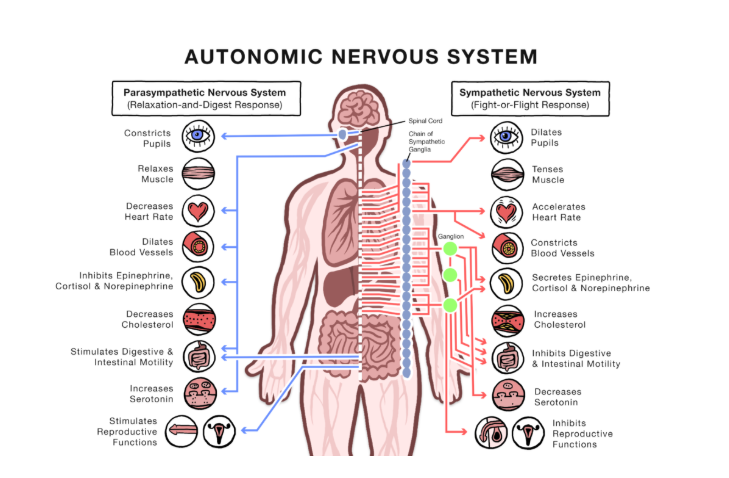
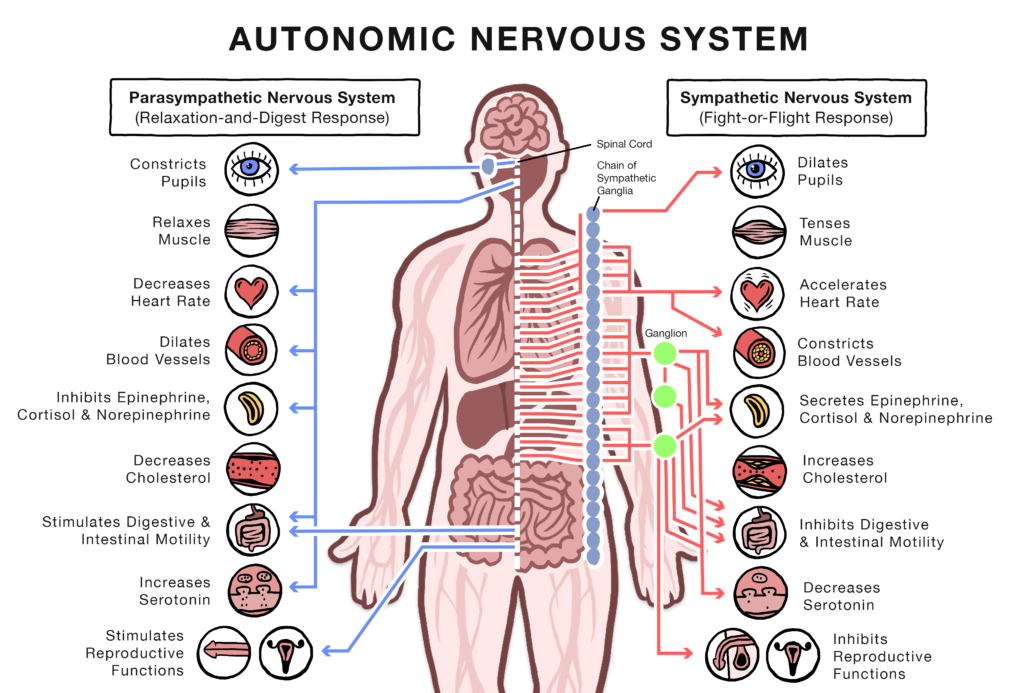
Dysautonomia is dysfunction of the autonomic nervous system (ANS), which regulates:
- Heart rate
- Blood pressure
- Temperature
- Digestion
- Immune signaling
- Stress response
When the ANS loses flexibility, patients experience:
- Lightheadedness
- Fatigue
- Brain fog
- Exercise intolerance
- GI dysfunction
- Sleep disturbances
The system becomes either stuck in sympathetic overdrive or unable to appropriately respond to stressors.
What Is POTS?
Postural Orthostatic Tachycardia Syndrome (POTS) is a subtype of Dysautonomia characterized by an excessive heart rate increase upon standing.
Common symptoms include:
- Rapid heart rate when upright
- Dizziness or near fainting
- Brain fog
- Fatigue
- Blood pooling in extremities
- GI complaints
While salt loading and compression garments can be supportive, POTS is rarely just a “volume problem.” It often reflects deeper autonomic, vascular, inflammatory, and connective tissue dysfunction.
What Is MCAS?
Mast Cell Activation Syndrome (MCAS) is a condition where mast cells release inflammatory mediators inappropriately or excessively.
Symptoms may include:
- Flushing
- Hives
- Itching
- Food sensitivities
- GI distress
- Headaches
- Brain fog
- Tachycardia
- Anxiety-like episodes
Mast cells exist throughout the body—especially in the gut, brain, skin, and blood vessels. When dysregulated, they amplify inflammation and autonomic instability.
The Overlap: Why These Conditions Travel Together
From our clinical experience, POTS and MCAS frequently coexist.
Here’s why.
1. Autonomic–Immune Cross-Talk
The autonomic nervous system regulates immune behavior. And your blood cells are connective tissues.
Low vagal tone → reduced anti-inflammatory signaling → increased mast cell reactivity.
Inflamed mast cells → histamine release → vasodilation → heart rate compensation → worsened POTS symptoms.
This creates a feedback loop.
2. Blood Flow & Vascular Instability
Histamine and inflammatory mediators alter vascular tone.
Excess vasodilation can worsen:
- Orthostatic intolerance
- Blood pooling
- Tachycardia
- Exercise intolerance
This makes POTS management incomplete without immune regulation.
3. Gut Dysfunction
The majority of mast cells reside in the gut lining.
Dysbiosis, increased intestinal permeability, or chronic stress can sensitize mast cells and disrupt autonomic signaling.
The gut becomes both a trigger and amplifier.
Axon’s Four-Lens Approach
1. Functional Neurology: Rebuilding Autonomic Flexibility
We assess:
- Heart rate variability
- Pupillary responses
- Oculomotor control
- Vestibular function
- Cerebral blood flow tolerance
Through targeted neurorehabilitation, we train:
- Vagal tone
- Brain connectivity
- Orthostatic tolerance
- Brainstem regulation
When the nervous system regains adaptability, both POTS and MCAS symptoms often decrease in intensity.
2. Functional Medicine: Reducing the Inflammatory Load
We evaluate:
- Gut health
- Micronutrient status
- Mitochondrial resilience
- Hormonal patterns
- Inflammatory markers
Interventions may include:
- Targeted nutrition plans
- Mast cell stabilizing nutrients
- Gut barrier support
- Mitochondrial cofactors
- Histamine modulation strategies
The goal is not suppression.
The goal is stability and resilience.
3. Physical Medicine: Structural & Mechanical Integrity
Mechanical stress influences autonomic tone.
Cervical instability, rib dysfunction, diaphragmatic restriction, and poor venous return can all exacerbate Dysautonomia.
Through:
- Precise chiropractic care
- Soft tissue therapies
- Breathing retraining
- Postural correction
- Progressive strength training
We improve mechanical efficiency and vascular return through strength.
4. Human Performance: Building Capacity, Not Just Avoiding Triggers
Many patients with POTS and MCAS have been told to “avoid overexertion.”
While pacing is critical early on, long-term healing requires rebuilding capacity.
We implement:
- Graded aerobic training
- Resistance training
- Blood flow tolerance drills
- Neurological resilience protocols
- Recovery optimization (sleep, light exposure, stress modulation)
Performance principles applied therapeutically restore confidence and physiological reserve.
A Small Highlight on Hypermobility
Many patients with POTS and MCAS also exhibit joint hypermobility.
Ehlers-Danlos syndrome (particularly hypermobile types) can contribute to:
- Vascular laxity
- Blood pooling
- Autonomic strain
- Chronic pain
- Proprioceptive instability
Loose connective tissue affects more than joints—it influences blood vessels, gut tissue, and structural support systems.
We’ll dive deeper into hypermobility and connective tissue disorders in the next blog.

The Bigger Picture
Dysautonomia.
POTS.
MCAS.
Hypermobility.
These are not random diagnoses.
They represent:
- Autonomic inflexibility
- Immune dysregulation
- Connective tissue vulnerability
- Metabolic stress
- Reduced physiological reserve
At Axon Integrative Health, we do not chase symptoms.
We restore systems.
When the nervous system stabilizes, inflammation decreases.
When inflammation decreases, vascular control improves.
When vascular control improves, confidence returns.
When capacity increases, life expands.
If You’re Ready for a Systems Approach
If you are navigating Dysautonomia, POTS, MCAS, or hypermobility and feel stuck in symptom management, there is another way.
Through Functional Neurology, Functional Medicine, Physical Medicine, and Human Performance, we help patients rebuild resilience from the inside out. Whether you’re a local, or would be traveling to see us, we will build a customized plan to help you reach your goals.
Your body is not broken.
It is dysregulated.
And regulation can be restored.